By Paul Schindler
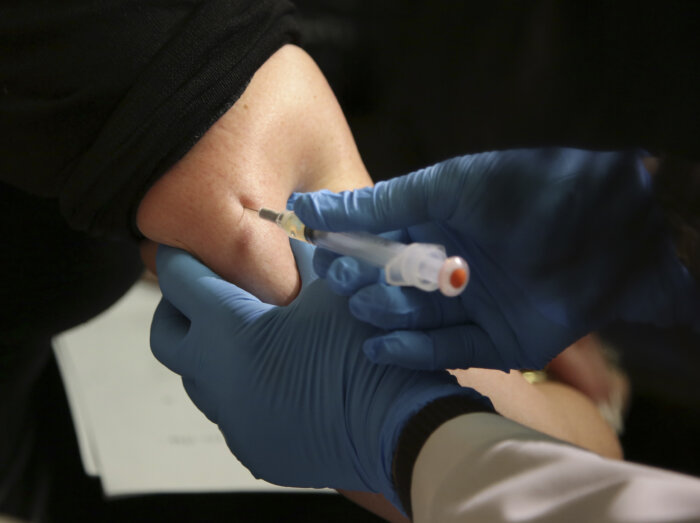
With COVID-19 cases surging to staggeringly unprecedented levels nationwide, a study of the HIV testing protocols in a hospital emergency room at the University of Chicago demonstrates the feasibility and the value of encouraging such testing even in the face of a crushing pandemic.
The university’s emergency room has prioritized routine HIV testing since 2011 because it represents an ideal location for identifying HIV diagnoses separate from those discovered in more targeted outreach efforts.
Efforts to end HIV/ AIDS as an epidemic rely, in part, on early diagnoses of the virus so that those infected can quickly begin treatment to reduce their viral load to the point where they cannot infect others even through condom-less anal sex contacts.
The study, published by the peer-reviewed journal AIDS and Behavior and covering the early weeks of the COVID outbreak in Chicago, noted that identifying individuals newly-infected with HIV, during which time they experience an initial acute infection stage where their virus is highly transmissible, is particularly important.
Patients in emergency rooms — arriving with serious symptoms they’ve never experienced before — are an important population to reach with HIV testing since the symptoms could indicate infection and, separate from such an ER visit, they might be unlikely to seek out regular medical care.
The onset of the COVID pandemic makes the emergency room all the more appropriate as a venue for HIV testing, the university ER leadership immediately recognized. Fears in the general public about COVID was driving up the number of people with influenza-like illness (ILI) to seek out emergency room care while those symptoms could instead indicate the acute infection state of someone newly infected with HIV.
Results reported in the AIDS and Behavior study covered the period from March 5 to April 18. A follow-up presentation by two of the study’s investigators at September’s Fast Track Cities Conference of the International Association of Providers of AIDS Care pointed to the success the university ER had in identifying a higher than typical number of acute HIV infections as it simultaneously tackled the COVID crisis.
In preparing for the expected arrived of COVID in Chicago, the ER set aside a large temporary space for patients presenting ILI symptoms but unlikely to require full hospitalization. Part of that planning involved incorporating HIV testing into the diagnostic work performed, which initially sparked some resistance from ER staff who felt that COVID needed to be the sole focus of their efforts given the enormity of that challenge.
Leaders in the ER, however, emphasized the similarities in symptoms between potential COVID cases and possible acute HIV infections, a message received well by those initially unconvinced, accord to the AIDS and Behavior study.
Outside of the temporary ILI evaluation space, the ER’s normal HIV screening efforts also continued.
In a virtual session at the Fast Track Cities Conference in September, two of the investigators — emergency medicine specialist Dr. Kimberly A. Stanford and infectious disease specialist Dr. David Pitrak — reported that the emergency room in the first eight months of 2020 identified nine cases of acute HIV infection. That compared to full-year results for 2016 through 2019 of seven, seven, four, and seven, respectively.
Asked during the virtual presentation to explain the ER’s increased identification of acute HIV infections, Stanford said, “I think one of the interesting things about COVID is that it is bringing people to the hospital seeking care who might otherwise not have come, so people who might otherwise have thought, ‘Oh, I have the flu, I have a cold,’ and stayed home, now they’re so scared that they might have COVID they are actually coming to the hospital to seek care and as a result this is our opportunity to screen them for HIV and oftentimes now we’re finding a few HIV cases in these suspected COVID cases.
She added, “This is, I think, highlighting why it is even more important than ever to continue our [HIV] screening efforts.”
The written study, published in May and covering the university ER experience in the earliest COVID phase through April 18, reported six HIV infections identified in the COVID testing area — including two acute cases. Most of those infected were young African Americans, three of them men who have sex with men, two cisgender heterosexual women, and one man who is an injection drug user. Five of the six were quickly put on treatment to bring down their viral loads, while the sixth had not reported back to the ER, as of the time of publication, for their follow-up visit.
According to the university investigators, “There should be no reduction in this important effort, even with the obstacles posed by COVID-19. While there are many obvious challenges to [emergency rooms] during the pandemic, there are also possible opportunities to reach patients who otherwise would not have sought care.”
The study also noted the fact that many other HIV testing venues were shuttered during the pandemic making the university ER all the more important as a location for identifying new HIV infections.
The conclusion from the University of Chicago investigators is that the ER’s model should be adopted around the nation — and with the tragic resurgence of COVID in recent weeks, that message couldn’t be timelier.
Last month, Amida Care, in partnership with Gay City News, hosted a webinar about the impact of the COVID pandemic on New York’s Plan to End AIDS. At the same time, Amida Care — whose Medicaid managed care plans deliver customized solutions for people living with HIV/AIDS as well as specific populations placed at higher risk for acquiring HIV, including people of transgender experience and those who are homeless — published a briefing paper on that subject.
The briefing paper drew particular attention to the lessons from the emergency room efforts at the University of Chicago, and Doug Wirth, the agency’s president and CEO, found the Chicago example critically important.
“Integrating routine HIV screening into emergency departments and other health care settings is critical to diagnosing newly transmitted HIV,” Wirth said in a written statement. “This is especially important given the heightened risk of transmission of acute HIV.”
This story first appeared on gaycitynews.com